Dengue & malaria (vector-borne)
Monsoon & post-monsoon (roughly July–November)
Breeding-site reduction, nets, repellents, and fever danger signs - test early and seek immediate care for severe symptoms.
Jan Ayush Sansthan works only in India. We run mobile and fixed-site health camps so screening, basic treatment advice, and awareness reach villages, wards, and campuses where distance or cost makes hospital visits rare.
Camps are run with local organisations, PRIs, schools, and volunteers. We prioritise diseases that matter here—conditions that are already widespread, seasonal, or rising in Indian states—and align with national programmes. Services follow ethical primary-care practice without replacing emergency or specialist care when it is urgently needed.


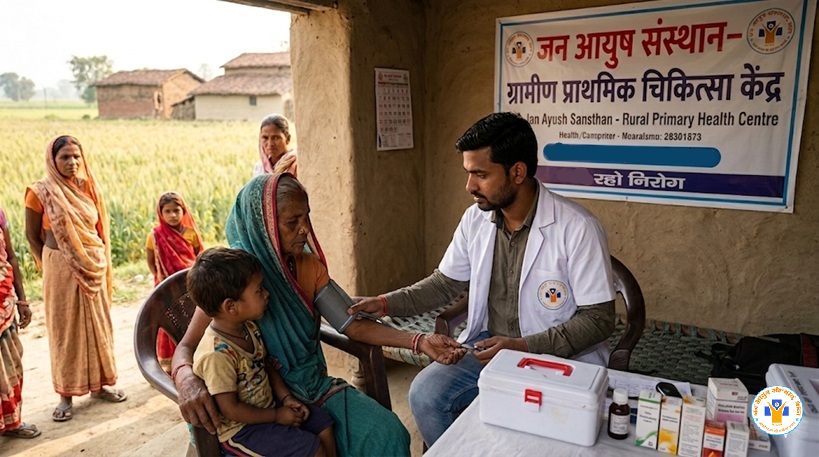
Blood pressure, random blood sugar where indicated, height–weight/BMI, and a structured general assessment—with clear advice on when to seek a doctor or hospital.
Essential medicines may be supplied strictly per protocol and local rules; focus remains on correct use, completing the course, and avoiding self-medication risks.
Short group and one-to-one sessions on hygiene, maternal and child health basics, non-communicable disease risk, and when to use government schemes and nearby facilities.

We plan each camp with local partners: permissions, publicity in simple languages, queue management, privacy for examinations, and referral slips or notes where follow-up is advised.
Priority is respectful care—especially for elders, pregnant persons, and children—and honest communication when a condition needs a higher centre.
Camps are scheduled where voluntary organisations and communities invite us—from tier-3 towns to peri-urban clusters. Geography changes; intent does not: reach families who otherwise delay care for lack of access, time, or awareness.
Villages and blocks where transport is costly; we aim for predictable dates, repeat visits where possible, and ties with ASHA/ANM networks.
Slums and dense wards where clinics are far or overcrowded; camps complement—not replace—municipal and state programmes.
Adolescent health, vision/hearing red flags, menstrual hygiene, and first-aid awareness tailored for students and staff.


Dates and venues are fixed with hosts several weeks ahead when feasible. Notices list what to bring (e.g. old prescriptions, ID), approximate timings, and any age-specific focus.
Camps are led or supervised by qualified clinicians and paramedics, with trained volunteers for registration and crowd flow. Protocols reference national guidelines; individual advice stays with the examining professional.
We emphasise documentation, respectful examination, and clear referrals. Trainees from Jan Ayush-affiliated courses may observe or assist under supervision where programmes allow.

Because our work is India-only, these 10 topic sheets focus on conditions communities are facing right now - seasonal outbreaks, high-burden infections, rising lifestyle disorders, and mental stress. Each page explains India-specific risky seasons, practical prevention, and clear what to do now action steps. They support national programmes and do not replace a clinician’s advice.
Monsoon & post-monsoon (roughly July–November)
Breeding-site reduction, nets, repellents, and fever danger signs - test early and seek immediate care for severe symptoms.
Year-round; cough >2–3 weeks needs testing
DOTS adherence, ventilation, and nutrition - do not stop medicines early; this is a critical step in TB control.
Often peaks after lean seasons & in young children
Complementary feeding, IFA, growth monitoring, and Anganwadi linkage - early action is important for children and women.
Lifelong; often silent until complications
Diet, daily activity, regular screening, and medicine adherence - early control is the best prevention for silent risk.
Summer & monsoon peaks; outbreaks after flooding
Safe water, ORS, hand hygiene, and child danger signs - quick response is essential to prevent dehydration.
Year-round; rising concern across Indian communities
Reduce stigma, improve sleep, and lower substance risk - seeking help from a counsellor is a strength, not a weakness.
Winter peaks; risk year-round in crowded settings
Fast breathing, chest indrawing, immunisation, and smoke-free homes - take the child to hospital immediately when red flags appear.
Birth dose & full schedule; antenatal protection
Safe injections, full vaccine schedule, and timely testing - prevention can significantly reduce future liver risk.
Often monsoon & harvest; snakes anytime
Immobilise, keep the patient calm, and transport quickly - avoid cutting or sucking; reaching an antivenom centre is the priority.
Summer heat waves; April–June in many states
Fluids, ORS, shade breaks, and quick action on heat red flags - treat confusion or collapse as an emergency and seek immediate care.
Share your proposed place, preferred month, and local partner—whether you need screening, topic-focused talks, or both. We will respond with feasibility, minimum requirements, and how responsibilities are shared between hosts and our team.